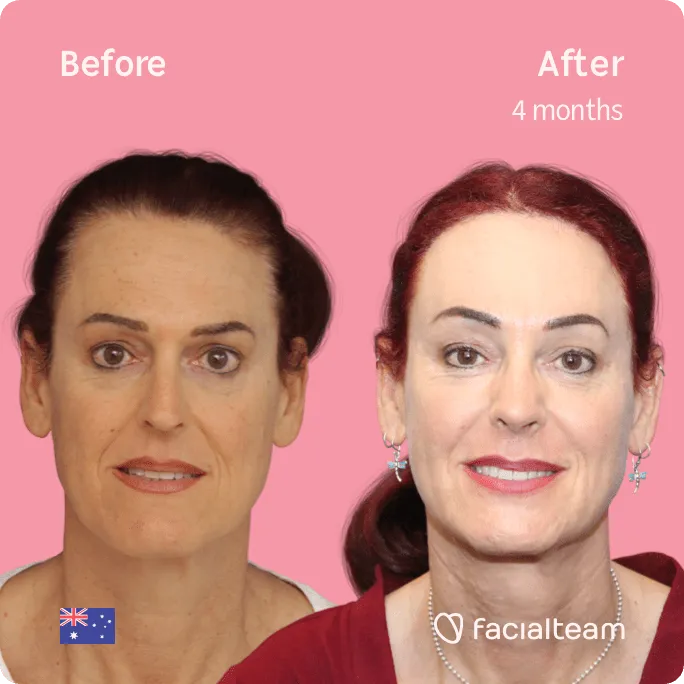
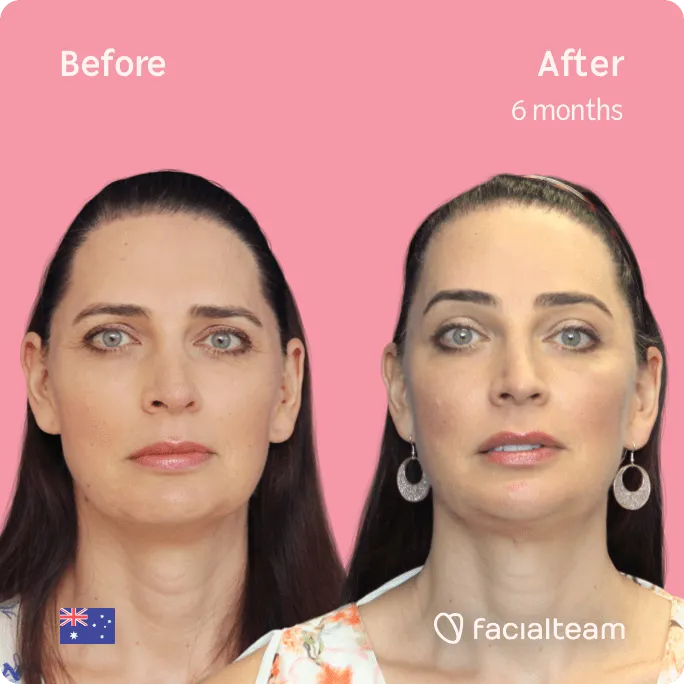
Hairline Feminization Surgery
Malin


Hairline Feminization Surgery is an umbrella term to describe redefining and reshaping the hairline for increased femininity.
So we can offer the best treatment for your desired look, we assess your hairline’s shape, height and hair density to define the best approach to obtain a feminine hairline.
This analysis will help you choose the ideal options for your unique case.
We determine the hairline height by measuring the vertical distance from between your eyes up to the center of the hairline. Hair density is calculated by dividing the number of follicular units (FU) per square centimeter on the scalp. (FU/cm2)
Facialteam has been trusted by over 943 hairline feminization surgery patients since the year 2008. We are proud to report extraordinary satisfaction rates, which inspire confidence in what patients describe as “high quality, life-changing results.”
Redefining Your Hairline to Match Your Feminine Identity
Hairline Feminization is optimal for people seeking to feminize their facial features. The hairline is influential in gender expression and can lead to being misgendered or not. There are several factors that influence the appearance of your hairline. Some common factors are:
- genetic inheritance;
- hormones;
- age;
- hair care routines;
- daily habits;
- prescribed medications.
All factors mentioned are addressed when undergoing hairline feminization surgery. When suggesting a solution, we consider these with the goal of achieving your desired look.
Hairline Feminization surgery contributes to an overall feminization of the face. Through this procedure you can achieve natural and lasting results. The course of action prescribed will depend on the aforementioned variables and your unique facial structure.
To better understand the obtainable results of hairline feminization, we explain how the hairline affects your gender expression.
Hairline Types
Our surgeons’ accumulated experiences have identified five distinct hairline types:
- Type I. Hairline with normal height and rounded format.
- Type II. Hairline with normal height and receding side temples, or M-shaped.
- Type III. A naturally high hairline.
- Type IV. High hairline due to alopecia (hair loss) with apparent temples.
- Type V. Undefined hairline due to advanced alopecia.
Depending on your hairline type, the treatment suggested could be with transplants or a hair replacement system. Read more to understand these methods and their effectiveness for different hairlines.
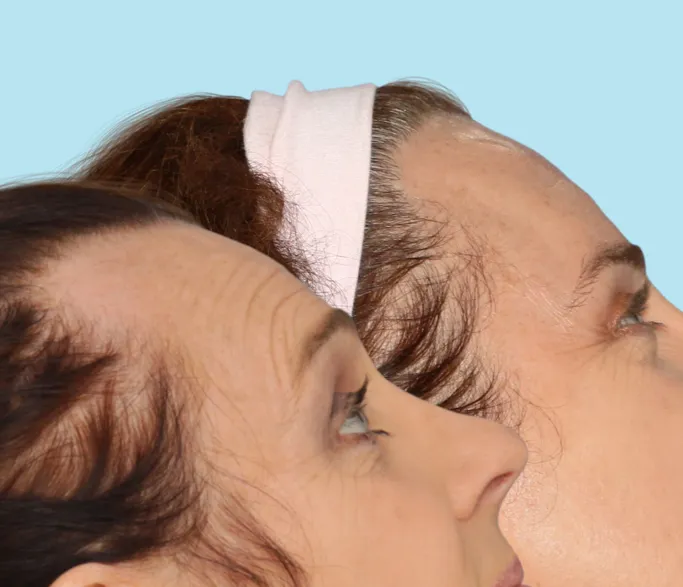
Differences between masculine and feminine hairlines
Masculine and feminine hairlines differ in their salient features. Masculine hairlines are generally further back on the scalp and have pronounced foreheads. This forms an M shape as the hairline recedes over time. The hair loss resulting in the M shape is recognized as a male forehead.
In comparison, a woman’s hairline seems to be closer to the eyes. However, it’s a common myth that women have shorter foreheads, despite the fact that many women have high foreheads without appearing masculine. In reality, a feminine hairline tends to be more rounded, creating an oval instead of an M.
The oval shape is what society reads as feminine and is the aim of hairline feminization surgery.
Methods of Hairline Feminization
There are three methods for completing a hairline feminization. They are mentioned below in order of most to least recommended:
- Hairline feminization with Hair Transplants (FUSS or FUE)
- Hairline Feminization with Hair Replacement System (HRS)
- Hairline Feminization with Hairline Lowering Surgery (HLS)
All methods of hairline feminization are effective, when indicated correctly, for creating feminized facial features. Here is an overview of the best method for the aforementioned hairline types.
With over 14 years of experience, our methodology, backed by the outcomes of over 943 successful procedures since 2008, has been recognized and acclaimed in renowned scientific journals.
Hair Transplantation (FUSS or FUE)
Hair transplantation focuses on recessed hairline areas that form an M shape. Therefore this procedure is ideal for patients with type II hairlines provided there is sufficient hair density and little or no androgenic alopecia. We employ two distinct techniques to obtain hair follicles, create hairlines and cover balding areas caused by alopecia.
The first technique is called follicular unit strip surgery (FUSS). In this method, we take hair follicles from a strip of scalp. FUSS is easier and quicker than the alternative technique, follicular unit extraction (FUE), which takes longer because we remove hair follicles individually.
If your hairline is type IV or V due to alopecia causing hair loss on the top of the head rather than the temples, hair transplants are a suitable solution. We can bring forward the hairline with sufficient grafts, for a lowering of up to 1 cm.
You can undergo hairline feminization using transplants before, during or after your FFS procedures. Let us explain with three scenarios.
- Simultaneous Hair Transplant during forehead feminization (SHT).
- Before facial feminization surgery.
- Delayed Hair transplant after facial feminization surgery.
We highly recommend the first option because it has many benefits. Simultaneous hair transplant is the best option for candidates who want combined forehead and hairline feminization. It limits the number of operations required for an optimal feminine result.
Simultaneous Hair Transplant (SHT) with Forehead Feminization
Simultaneous Hair Transplant (SHT) is a technique developed by Facialteam through research and experience. There are three stages involved in the process.
First, dermatologist surgeons identify the best donor area of the scalp. We then preserve the strip of scalp that is removed in the modified coronal approach in order to access the forehead region. Next, hair technicians harvest and prepare the hair follicles in different units. Finally, we design a new hairline by grafting the segmented follicles along your new forehead.
All stages are completed in succession and simultaneously in one operation.
For your safety and to reduce risks associated with prolonged general anaesthesia, we wake you up and use light sedation during the hair grafting stage. This ensures the operation is pain free and performed to the highest safety standards.
If you have androgenic alopecia, it should be stabilized before performing SHT. If hair loss is significant, we can adjust incision positions from the crown to a position further back on the scalp. If necessary, we may even create the incision on the back of the scalp.
SHT has its limitations, which include a maximum number of harvestable hair follicles and covering balding temples with full density. If needed, we recommend a second hair transplant a few months after SHT.
Hair Transplants Before FFS
Some candidates prefer hair transplants to feminize their hairline before FFS.
If you want hair transplant surgery before FFS, it is recommended to wait at least a year before further operations. This will allow your body time to heal and guarantee that hairline grafts are settled. It maximizes the use of hair follicles and secures their viability if they are needed again.
This option is less desirable than SHT due to the waiting times.
Delayed Hair transplant after facial feminization surgery
Some patients delay hair grafting to a separate post-operative session. You may opt for a FUSS or FUE technique.
If you choose delayed hair transplants, you should wait a minimum of 6 months after FFS procedures. This delay time is important so that your face is properly healed and all swelling and bruising are gone. Full consolidation of the soft tissues in operated regions of your face during FFS procedures recreates the ideal environment for hair grafts.
This option requires two surgeries and longer waiting times than SHT.
Stages of Hair Transplant Growth
Undergoing a hair transplant can be a life-changing experience. However, the recovery process is a gradual one, and patients should be prepared for a series of stages as their hair grows and their scalp heals.
We will explore the different stages of recovery after hair grafting, from the initial days to the final result months later. Understanding the different phases can help you manage expectations and ensure the best possible outcome for your hair transplant procedure.
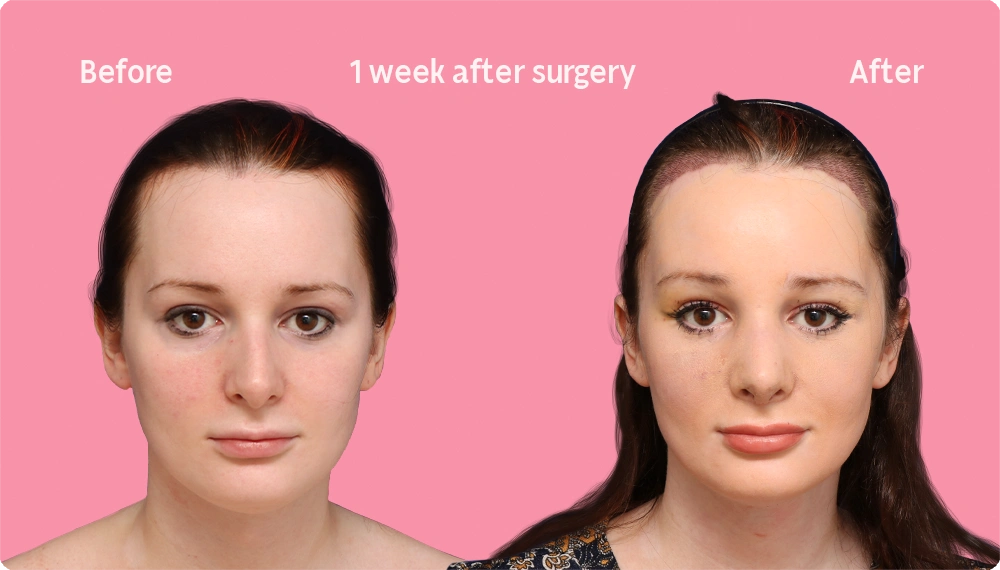
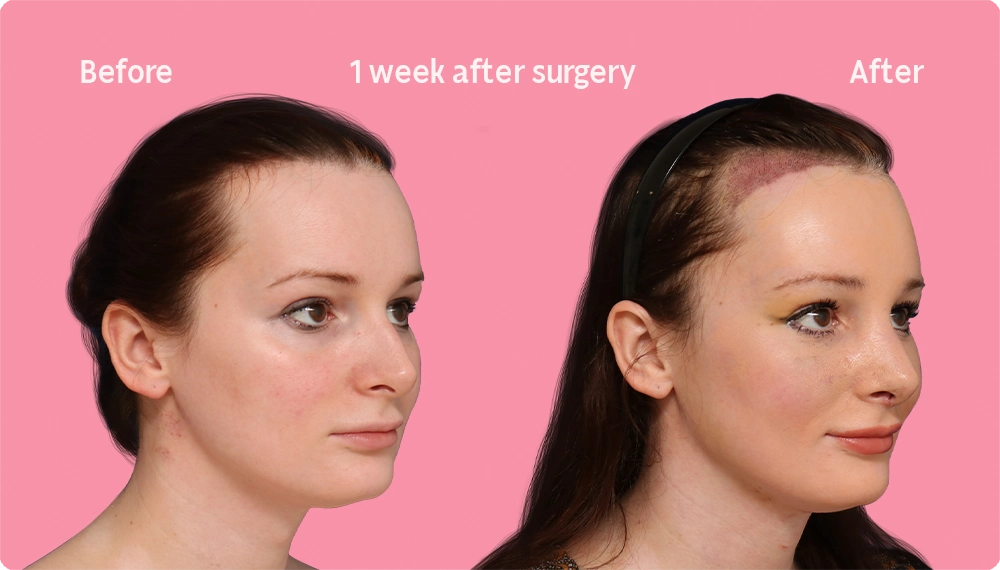
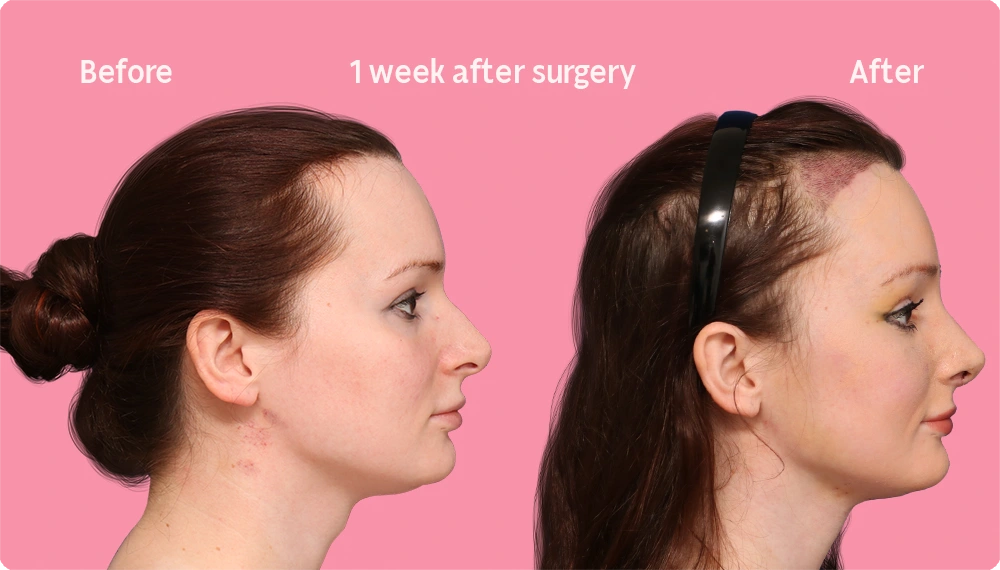
Hair Transplant Growth in the first week
After a hair transplant surgery, the first hair wash is a crucial step in the recovery process. Within a few days or weeks, it is completely normal for the ends of the hairs to fall off, leaving behind “pilot stems.” The skin may also redden as the healing process drives blood flow to the tissues.
Patients may feel some discomfort, such as itching or tenderness, which can be managed with medications and topical aftercare. Follow the instructions provided by the hair transplant surgeon strictly to minimize symptoms.
It is important to avoid rubbing or scratching the scalp during this stage, as this can damage the newly transplanted follicles or cause infections that impede the healing process. Use the nutritional and hair care products as recommended by the specialist to create the ideal conditions for the grafts to settle and grow into healthy hair.






While the appearance of the skin and the apparent disappearance of the hairs at this stage may be somewhat disconcerting, it is important to remember that this is a normal part of the healing process.
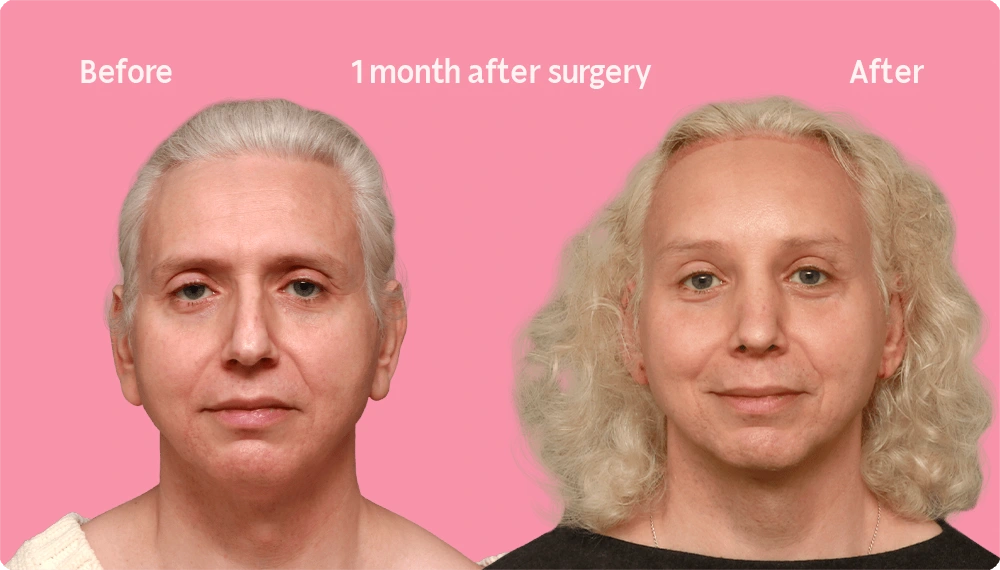
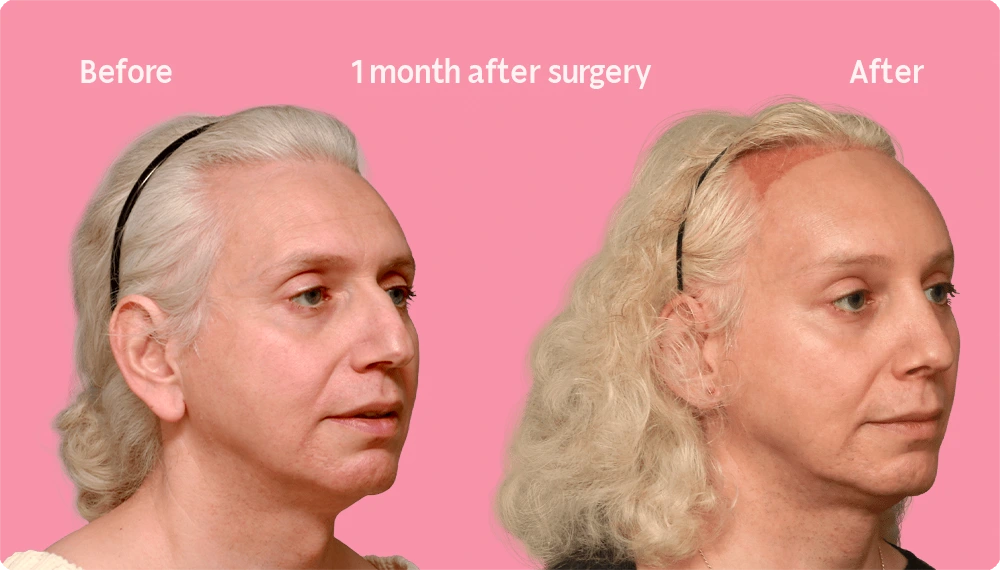
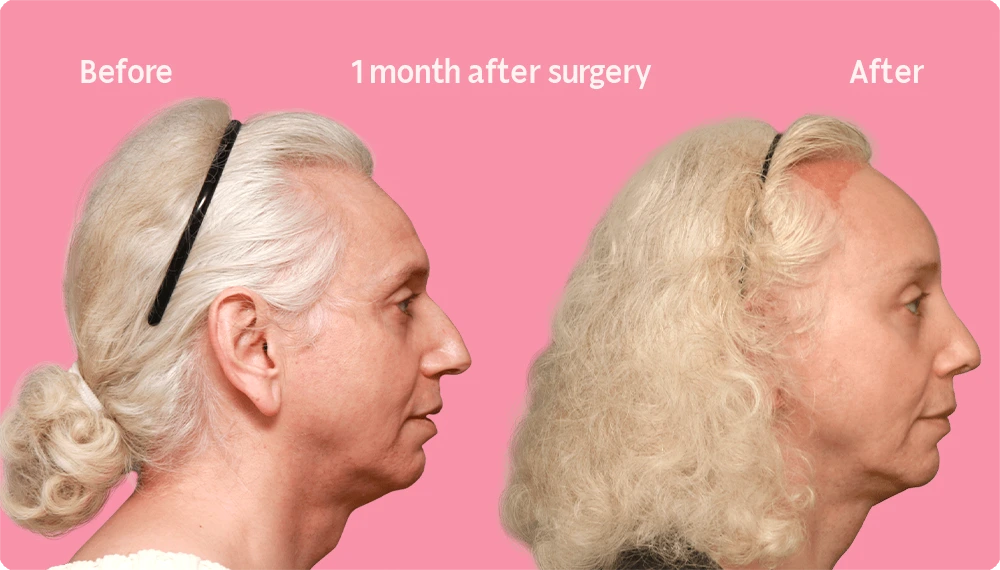
Hair Transplant Growth after 1 Month
As seen in the before and after images of this patient, 1 month after undergoing a hair transplant, it is common for most of the ends of the transplanted hairs to “fall out” during the initial phase.
Do not be alarmed as new hair growth will begin in the following months. The recipient area which appeared pink or red gradually subsides and returns to its normal skin tone.






The initial phase of a hair transplant may seem discouraging as it is a gradual process that requires patience and careful maintenance. With proper care you can expect to see a significant improvement in your hair growth and appearance.
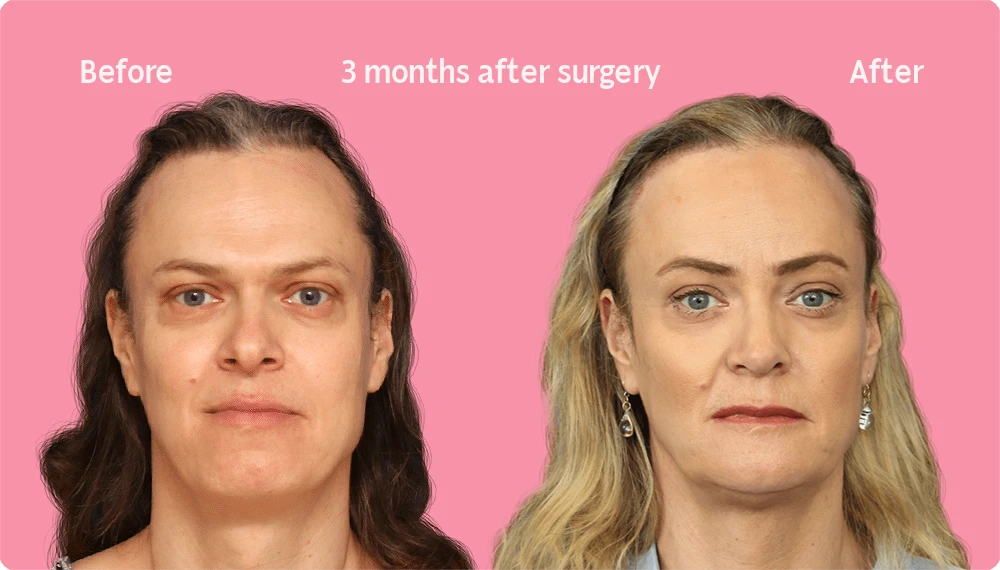
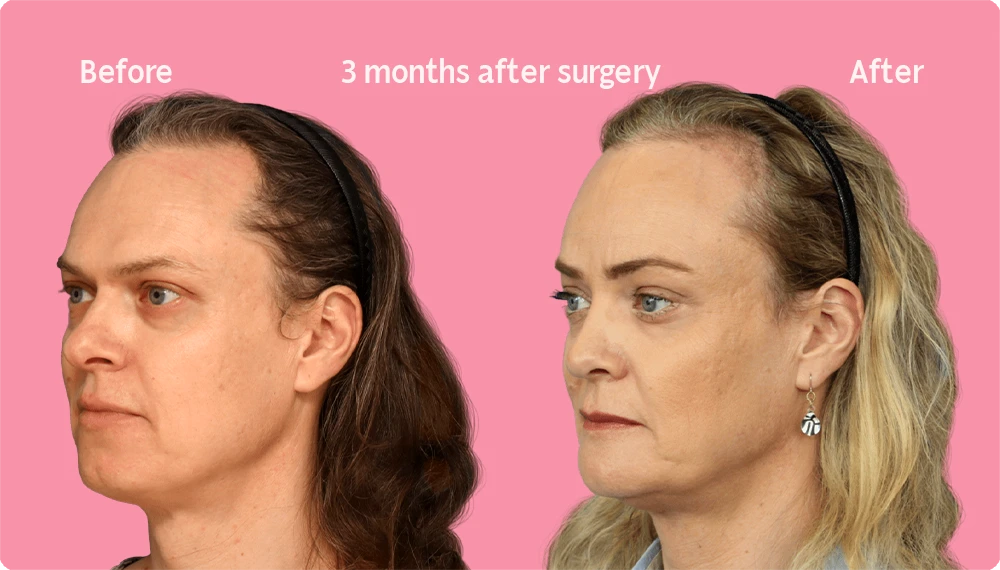
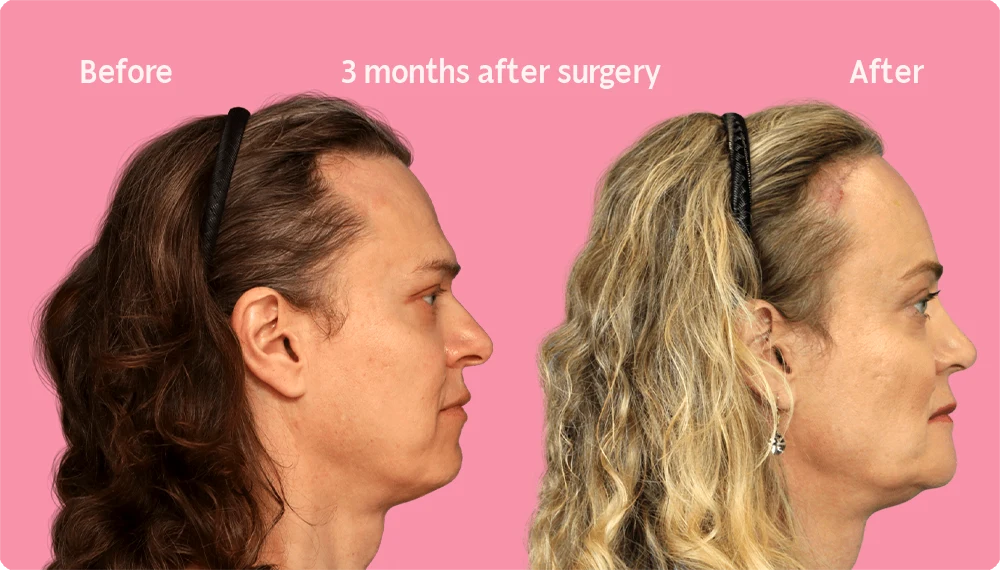
Hair Transplant Growth after 3 Months
Three months after a hair transplant, the first signs of new hair growth begin to appear. Although the number of sprouting hairs is still relatively small and they may appear thin, this early growth is a sign of the success of the procedure.
Keep up the diligence in your aftercare habits to encourage more baby hairs to emerge.






Over the coming months, the newly transplanted hairs will begin to thicken and more will appear. This gradual evolution will eventually result in a significant improvement in your hair density and appearance, as the case images show.
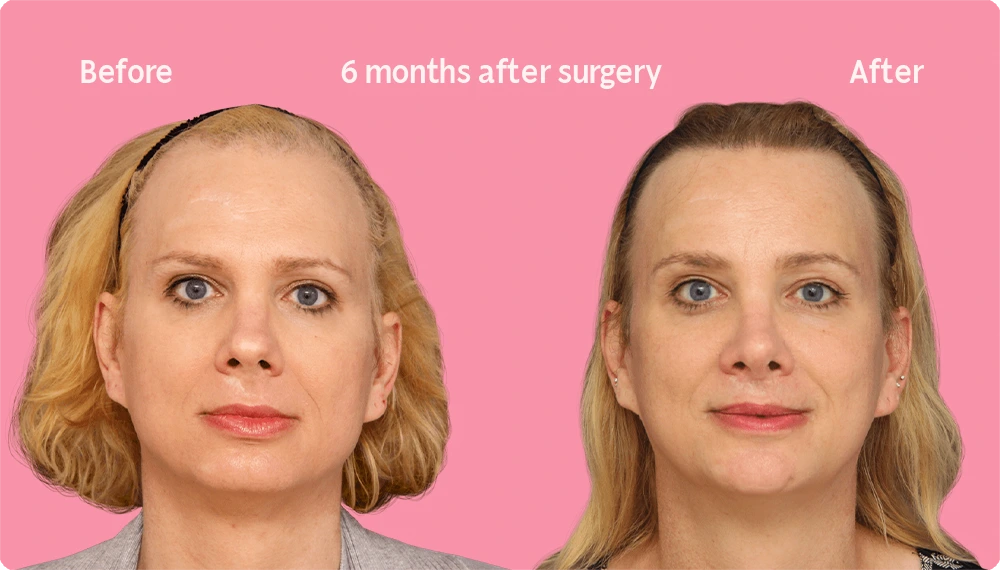
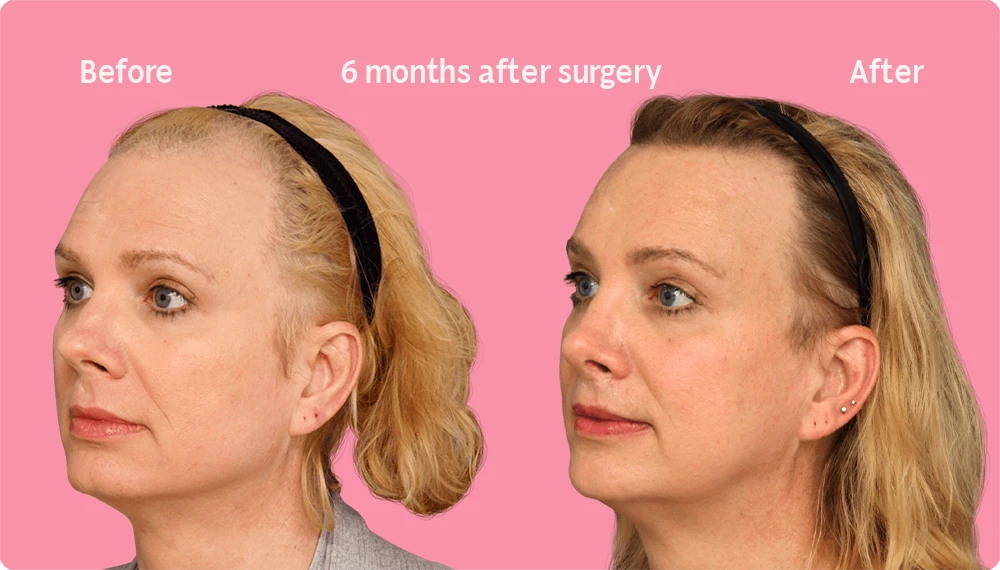
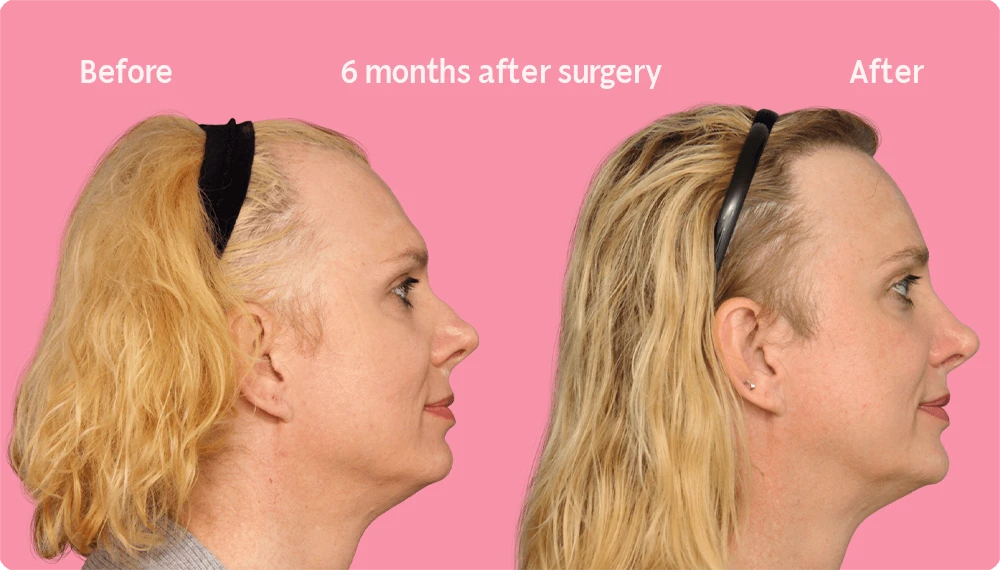
Hair Transplant Growth after 6 Months
At the six-month mark after a hair transplant, a high percentage of the follicles have already grown. While the result at this stage of the recovery process is quite advanced, although the definitive result yet to come. This is due to the normal regrowth and loss cycles typical of human hair follicles.
The remaining hairs that have not yet emerged will continue to do so. The thickness of the baby hair shafts will improve. Slowly but surely, the transplanted area blends in with the rest of your hair.






While the full results of a hair transplant may take a year or more, the patient can feel encouraged by the progress made thus far.
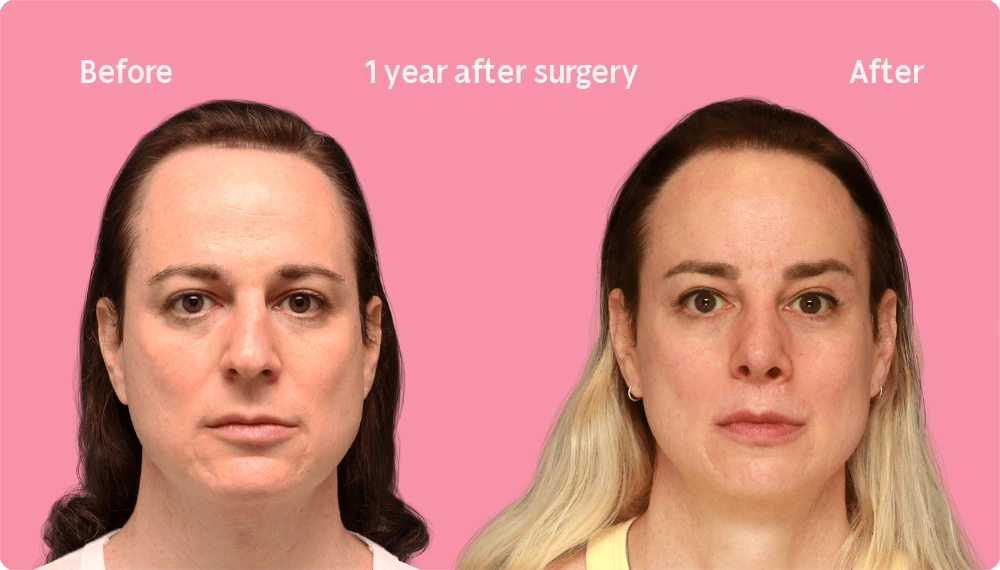
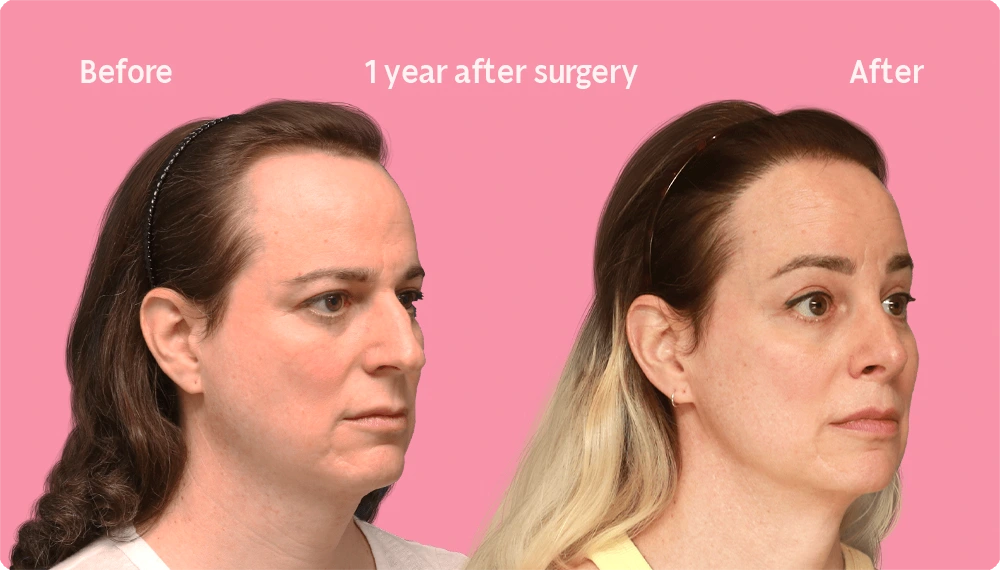
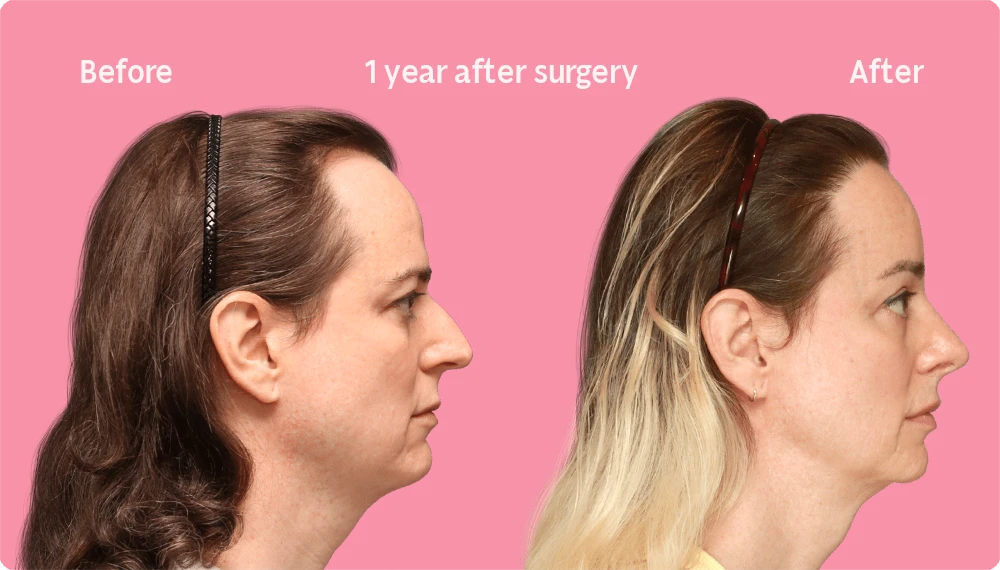
Hair Transplant Growth after 12 Months
After 12 months, the final result of a hair transplant is practically complete. All of the transplanted hairs have appeared and most have reached their final thickness, resulting in a positive difference in your hair density and appearance along the hairline.
At this point, you may judge the success of the procedure and are likely enjoying the restored hair for a more feminine hairline shape. Regardless, don’t forget to continue the care instructions to protect the young grafts as they develop into healthy and long hairs.






A successful hair transplant can be a life-changing procedure for patients who have struggled with hair loss. With proper care and patience, the patient can expect to enjoy the benefits of their restored hair for many years to come.
Hair Replacement System (HRS)
The Hair Replacement System by Cesare Ragazzi Laboratories is non-invasive and can fully or partially restore beautiful hair seamlessly on the scalp.
The Hair Replacement System is best for patients with extreme alopecia leading to an undefined hairline (type V).
The HRS replaces lost hair by means of a dermatologically-tested clone membrane or “second scalp” personalized for your unique hair characteristics. The second scalp is made from selected human hair then hand-woven onto a high-quality and comfortable base. It is designed to match your hair’s features such as density, contour and flow.
Integration with medical-grade adhesive allows for maximum comfort and breathability.
The HRS is designed and integrated with your scalp in seven phases.
- Scalp mapping: computer mapping of the scalp and alopecic area.
- Cast production: cast created using specialist computer imaging, cloning the contours of the skull and scalp.
- Cloning and pantone matching: clone membrane created by robotic technology, replicating the exact shape, lines, and skin tone of the patient’s scalp.
- Hair selection and matching: meticulous selection of high-grade human hair to replicate colour and texture.
- Implanting: the hairs are implanted individually into the membrane, mirroring the original direction of growth.
- Non-surgical grafting: the membrane is non-surgically grafted onto the scalp.
- Final styling: professionals complete a final styling as the HRS system is fully integrated.
Since the HRS is non-invasive you can return to normal life without restriction after integration with your scalp. The system includes a personal care consultant who will clean and style your beautiful new hair monthly.
Hairline Lowering Surgery (HLS)
Hairline Lowering Surgery (HLS) is a technique of hairline feminization. This procedure is not recommended for most patients. There are some disadvantages to this technique, which include possible visible scarring, unnaturally small foreheads and inability to improve the hairline shape effectively. These limitations unfortunately may require additional interventions or cosmetic treatment in order to obtain optimal results.
So, the use of this technique is rare.
In our years of experience, only 1% of all patients need this surgery. This technique is used for severe cases of alopecia on the temples (hairline type IV) and unnaturally high hairlines (hairline type III).
In HLS we remove a strip of skin from the forehead and advance the scalp 1 to 2 cm. We carefully make an incision approximately 2 mm inside the hairline behind the implantation line. The incision is placed here so that potential scars are less visible.
This procedure has two benefits. First, it reduces the excess height of the forehead. After the procedure, the distance between your hairline and eyes will fall within more feminine parameters. In addition, we may reconstruct the frontonasoorbital complex in the same session, feminizing all the bone structure in the eye orbits, brow and forehead region.
How much does Hairline Feminization Surgery cost?
The price of Hairline Feminization can vary, as the combination of diagnostics, techniques and procedures are personalized to your particular situation. The overall costs for Hairline Feminization Surgery with Facialteam (including hospital fees and anesthesia) may range anywhere from 7 900 € to 8 500 €. Depending on the details of complexity and if you choose optional aspects, the final cost may be higher or lower.
The following services are included in all our quotes;
- pre-operative consultation, standard pre-operative preparations and necessary revisions;
- preoperative and postoperative CT-scan;
- material costs;
- costs for the operating theater and general anesthesia;
- 1 night in hospital;
- lymphatic drainage massage;
- acupuncture service;
- 24-hour coordination support;
- post-operative nursing care;
- health insurance for surgical complications up to 30 days after your surgery.
We suggest consulting with several surgeons, whose approaches will vary, in order to make a more informed decision of what is best for you.
Consultations
There are various approaches to hairline feminization. The suggested procedures will depend on your unique hairline characteristics. Our analysis of your case will help you determine the best options for your facial feminization goals.
Consultations will provide the information you need to be well-informed about your facial feminization journey. They are always free.
We care about your journey and want you to know everything about the procedures you will need for your desired look. At our clinic we are equipped with the latest technology in order to provide the most accurate recommendations in your case.
During the consultation we will talk about your goals together to create the optimal plan for you.
Book your Consultation
We offer both online as in-person consultations in our clinic in Marbella, Spain. Our consultations are free of costs and a great aid for those patients seeking advice to start their journey.
Frequently Asked Questions
-
Minoxidil
Minoxidil applied in non-transplanted areas, works like finasteride/dutasteride (although it is less potent than these), that is, preventing the progression of alopecia. However, applied in the transplant area after 6 weeks, it has been shown to accelerate the growth of the grafts.Finasteride & Dutasteride
Based on your specific case (type of alopecia, medication taken etc.), the specialist may have decided to prescribe finasteride or dutasteride to prevent progression of alopecia, avoiding the need for a second transplant in the short term.These medications can help to prevent progressions of alopecia to avoid a second transplant in the short term.
-
We recommend these instructions for our patients, if you’re in doubt, please contact your treating doctor.
- Day 1
Use Saline Solution during the first 7 days, every 30 minutes, on the recipient site, wetting the area well to keep it moist. At night, do it only when you wake up anyhow. To apply the Saline Solution, spray it with a dispenser from a slight distance, without directly touching the recipient site. Doing otherwise could create a scab that will prevent the hair from growing. If you run out, you can refill the dispenser with Saline Solution or consult your coordinator if you prefer. - Days 2 to 7
Continue keeping the grafts moist with Saline Solution, every 30 minutes. Besides, from day 2, apply Betadine Shampoo directly to the recipient site using the dispenser. Apply it gently, without massaging or touching the recipient site. When rinsing the area, the water pressure should be very low or you can use a small cup of warm water. Follow these instructions once per day:- Spray Betadine Shampoo on the hair transplant area;
- Leave it for a minute and then rinse it out;
- Repeat this process 3 times.
Note: You should also wash the incision area with Betadine Shampoo. - Apply rosehip oil directly over the recipient site every night before going to bed.
- Days 6 – 7 after the transplant
Our nursing staff will wash your hair. - Days 7 to 8 after the transplant
Continue applying Betadine Shampoo to the transplant site (even though there were no scabs), begin to gently massage the scalp with your fingertips in a circular motion, using normal water pressure to rinse. If you wish, you can also use a gentle shampoo like Triconails Shampoo by Cosmeclinik after using the Betadine Shampoo. Continue to wash your hair 1 or 2 times a day. On the day of the final revision, the postoperative coordinator will give you further instructions. - Days 8–14 after the transplant
Continue applying Betadine Shampoo to the transplant site (even though there were no scabs), beginning to gently massage the scalp with your fingertips in a circular motion, using low to normal water pressure to rinse. If you wish, you can also use a gentle shampoo like Triconails Shampoo by Cosmeclinik after using the Betadine Shampoo. Continue to wash your hair 1 or 2 times a day. If you do not have any more scabs, one time per day is enough. - Day 15 after the transplant
If you have followed the postoperative instructions correctly, you should not have any scabs. You can use the Cosmeclinik, a baby shampoo or a normal mild shampoo to wash your hair. Be gentle when touching and avoid any hit on the area. In case of crusts, you can apply a little amount of olive oil to the area one hour before washing your hair to soften the site. - 1 Month after the transplant
We recommend using a mild shampoo as long as possible unless you feel that it does not work for you. In this case you can start using your usual shampoo. Make sure that it is not aggressive or strong. Also, you can now wash your hair normally. If you have a dermatitis outbreak, please let us know and we will give you specific instructions.
- Day 1
-
It is extremely important to not touch the transplant area during the first 7 days after your hair transplant.
-
During the first 6 weeks, you should cover the transplanted area and prevent it from direct sun exposure.
In the first 6 months, you should avoid any sunburns on your scalp.
-
Swimming in natural waters
We recommend waiting 1 month before diving in with your head in the sea or other natural water.Swimming in a pool
Wait 3 months before diving in with your head in a pool, due to the chlorine. -
Hair coloring with dye
Avoid the transplant site until 3 months after surgery.Hair coloring with capillary fibres
These should not be used until 6-8 weeks after your surgery.
Research & Education in Hairline Feminization Surgery
Facialteam’s R&D group has established a new framework of modern protocols in FFS of the forehead and hairline. For us, advancements in science translate into offering our patients the very best in facial gender surgery, with natural looking results and quicker recovery times.
Publications
This technique is based on several scientific articles produced by our group throughout our clinical practice. Our academic literature is a record of our dedication to the science of feminization surgery of the upper facial third since 2008.

Facial Feminization Surgery: Simultaneous Hair Transplant during Forehead Reconstruction

The Upper Third in Facial Gender Confirmation Surgery: Forehead and Hairline