Your Journey to FFS Surgery with Facialteam
Embarking on the transformative path of facial feminization surgery is a significant decision, filled with anticipation, questions, and emotions. At Facialteam, we recognize the weight of this journey and the importance of clarity and support.
Our mission is not just to provide world-class surgical expertise but also to guide, inform, and stand by you at every phase. From the initial consultations, through the intricate details of the surgery, to the post-operative care and beyond, we’re dedicated to ensuring that every patient feels understood, prepared, and confident.
This journey is as much about personal discovery as it is about physical transformation, and we’re honored to be your chosen partner. Dive in to get a comprehensive overview of what your journey with us will encompass.
Preparing for Your Journey
Embarking on the path of facial feminization is a significant decision, marking a bold step towards aligning your physical appearance with your true identity. As you prepare for this transformative journey with Facialteam, it’s essential to be well-informed and confident every step of the way.
The period before your arrival is a time for education, consultation, and thoughtful preparation. It’s a time to gather all the necessary information, understand the procedures, and set realistic expectations for the outcomes.
We are committed to providing you with all the resources, support, and guidance you need during this crucial phase.
Our dedicated team is here to answer your questions, address your concerns, and ensure that you are mentally, emotionally, and physically prepared for the surgery.

Educate yourself
Start by determining if FFS is the right choice for you. Delve into critical discussions about Gender Dysphoria and its connection to Facial Feminization. Hear firsthand from our past patients, such as Eunice, and learn about their life-changing experiences with us.
Preparing for surgery with Facialteam also means preparing for your recovery. From the very beginning, your coordinator will help you plan every stage of your stay, including your post-surgical experience at Naghoi, our new sanctuary for recovery.
This early planning ensures that your healing journey begins even before your surgery day.
Revealing Eunice: The Complete FFS Journey Video Experience
In this intimate and groundbreaking documentary, we follow Eunice before, during, and after her life-changing surgery at our renowned Marbella, Spain clinic. Experience a complete Revelation Journey and the emotional and physical transformation as we dive deep into the world of FFS, addressing common fears and misconceptions.
Gain insight into the unwavering support system that Eunice and other transgender individuals rely on during this transformative chapter of their lives, highlighting the profound impact of compassionate care and authentic self-expression.
Choosing the Right FFS Surgeon
Understanding Facial Gender Confirmation Surgery is crucial. We’re here to help you find the best FFS surgeons tailored to your needs. With transparent information and heartfelt patient testimonials, we aim to make your decision-making process on choosing the right ffs surgeon as informed as possible.

Who Performs My Surgery At Facialteam?
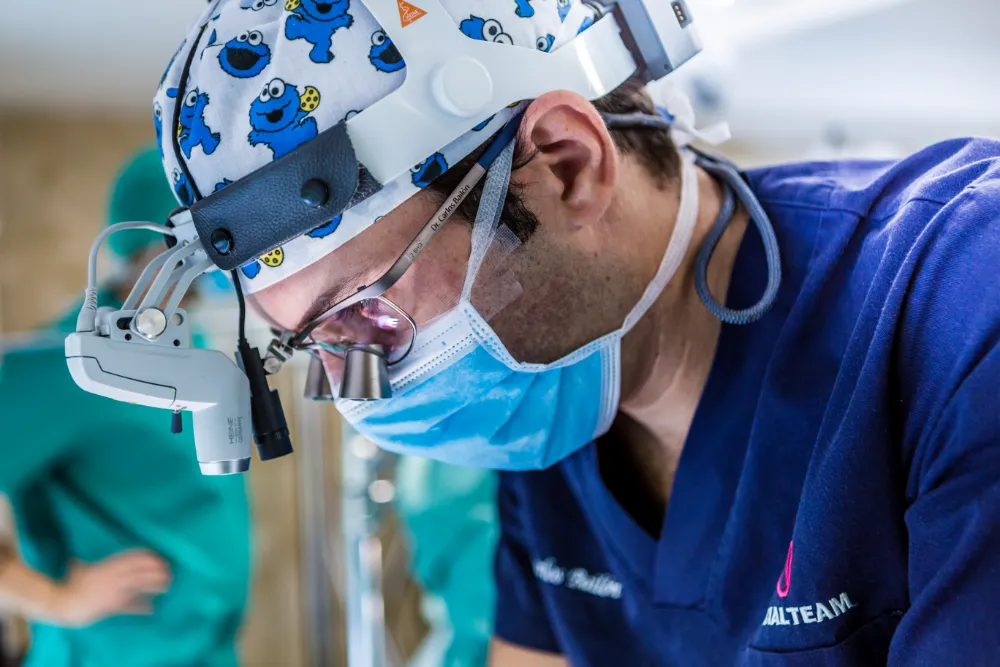
Best FFS Surgeons: What to Know and Where to Go
Consultation
Before diving into the transformative process, it’s crucial to have a comprehensive consultation. This session serves as an opportunity for you to discuss your goals, understand the procedures, and get a clear picture of the expected outcomes.
Although some clinics or surgeons charge a fee for a consultation, we always recommend to speak to several surgeons to identify who you feel most comfortable with. Consultations at Facialteam are always free and are offered both online and in-person in Marbella, Spain.
Whenever possible, we highly recommend visiting our center in Marbella in person for your consultation as it provides a complete preview of the Facialteam experience:
- A comprehensive 1-hour consultation with one of our FFS surgeons to discuss surgery details and address your questions.
- Immediate quote delivery and consultation with a Patient Coordinator.
- Firsthand experience in HC International Marbella Hospital, where Facialteam is located
- High-quality images for your consultation captured in our in-house studio using professional-grade cameras, lighting, and backgrounds.
- The opportunity to meet Facialteam’s staff in person before undergoing surgery.
- A live Virtual Facial Feminization Surgery (VFFS) simulation by our VFFS expert, to see a realistic post-surgery facial outcome.
- 3D CT-Scan for in-depth analysis of your facial bone structure, enabling more precise surgical recommendations.
- Airport transfers to and from Málaga Airport.
- The possibility of attending group sessions led by our Psychologist, if available during your stay.
The entirety of this comprehensive package, if quantified, has an estimated worth of over 600 euros. Despite its immense value, we at Facialteam are pleased to offer it to our patients absolutely free. It’s our way of ensuring that you receive the best insight, experience, and care, even before you take the step towards transformation.
Exclusive Offer: Don’t Miss Out!
The value of our comprehensive consultation package speaks volumes, and we’re offering it to you absolutely free. With a combined worth of over 600 euros, the slots are in high demand. Act now, and ensure you’re ahead of the curve, getting the most detailed insights and unparalleled care before your transformative journey begins.
Before Arrival: Planning & Preparations
There’s a lot to consider before your surgery. From administrative tasks to health documentation and essential tests, we’ve got you covered. Our dedicated coordinators are on hand to offer a personalized patient guide and a comprehensive schedule, ensuring you’re ready for the journey ahead.
As part of this step, your coordinator will share details about your upcoming stay at Naghoi, including medical follow-up, psychological support, and the serene environment designed for your recovery.
Knowing what awaits you after surgery helps you prepare not only logistically but emotionally.
During Your Stay: Your Surgery Experience
Your time with Facialteam is more than just a surgical procedure; it’s a holistic experience designed with your comfort and well-being in mind. From the moment you arrive to your recovery phase, every detail is meticulously planned to ensure you feel supported and cared for.
Arrival
Begin your journey on a positive note. Upon arrival, our trusted drivers will welcome you and transport you seamlessly to your accommodation in Marbella.
For patients undergoing surgery in Marbella from 2026 onward, Naghoi will be your home during recovery. This purpose-built recovery center was created exclusively for Facialteam patients, offering a peaceful, private space with professional nursing, psychological care, and wellness services.
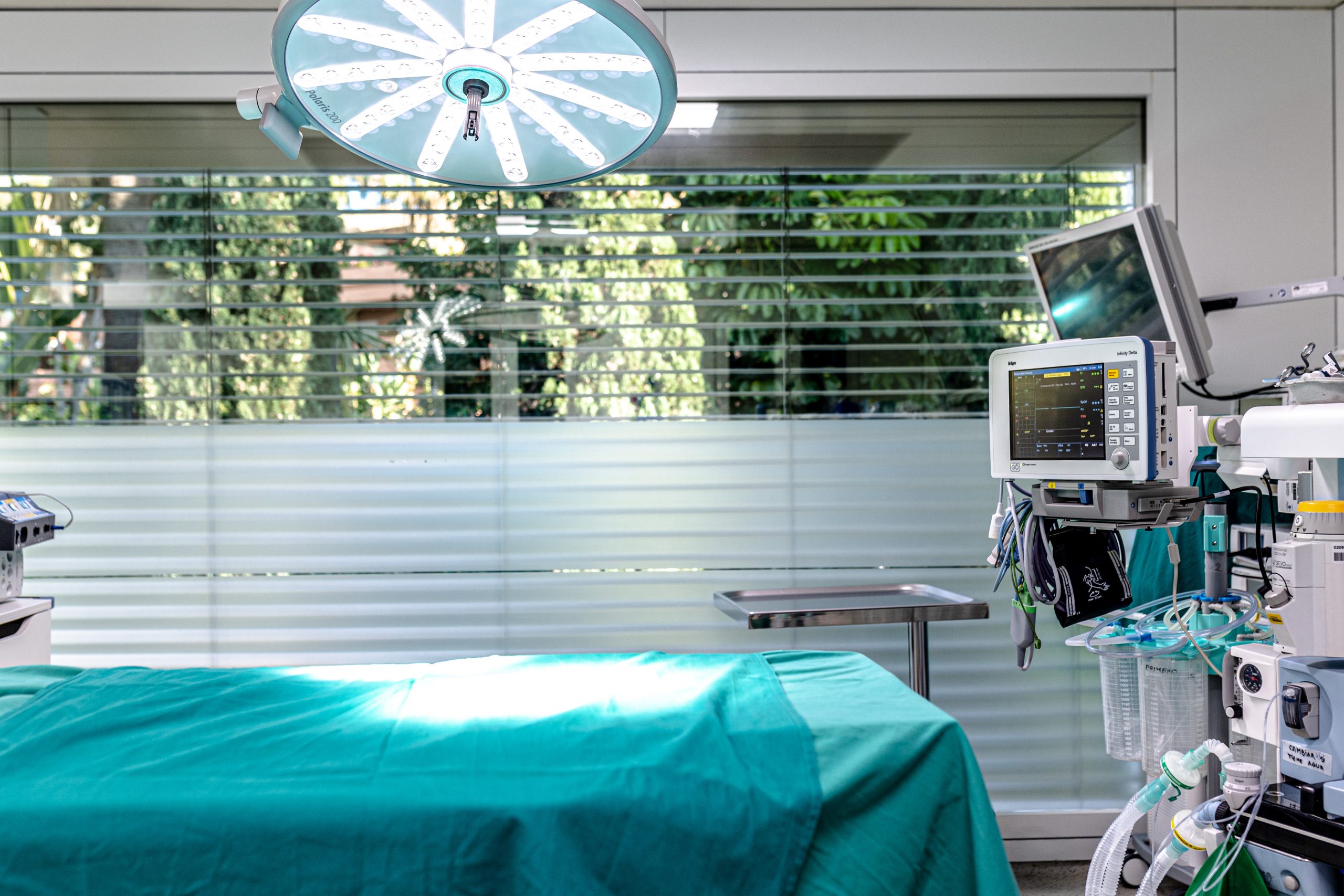
Pre-Op Evaluation
Depending on when you arrive, you’ll embark on the preoperative FFS process. This includes health interviews, an electrocardiogram, clinical photo sessions, and 3D CT scans. This thorough evaluation ensures we’re fully aligned with your needs and concerns.
Day of the Surgery
Your big day is orchestrated to ensure utmost comfort and clarity. From admissions to post-surgery care, your dedicated patient coordinator will be by your side, guiding you and ensuring you’re well-informed every step of the way.
Recovery & Aftercare
Your well-being post-surgery is our priority. Benefit from our comprehensive care system, which includes psychological support and advanced treatments like hilotherapy and lymphatic drainage, all aimed at facilitating a swift and comfortable recovery.

Recovery at Naghoi
After surgery, your recovery continues in Naghoi, Facialteam’s new post-operative recovery sanctuary for trans and gender-diverse patients.
Born from over 15 years of experience, Naghoi was designed to provide a safe, serene, and healing environment where you receive:
- Daily nurse visits and medical supervision
- Individual and group psychology sessions with gender-specialized therapists
- Lymphatic drainage and acupuncture for comfort and balance
- Nutritious meals designed for recovery, made with local ingredients
- Private rooms with smart technology and adjustable beds
- 24/7 support, transfers, and a caring, inclusive community
Naghoi represents the heart of the Facialteam experience —where science meets empathy, and recovery becomes a deeply human process.
Accommodations
For surgeries in Marbella from 2026 onward, Naghoi will offer a fully integrated environment where every aspect of comfort, privacy, and healing has been reimagined.
Your journey with Facialteam is a blend of medical excellence and heartfelt care. We’re dedicated to ensuring that your stay with us is as comfortable, informed, and positive as possible.
Back Home: Post Operative Support & Care
Traveling back home marks the beginning of a new chapter. While the surgical procedures are complete, our commitment to your recovery and well-being continues.
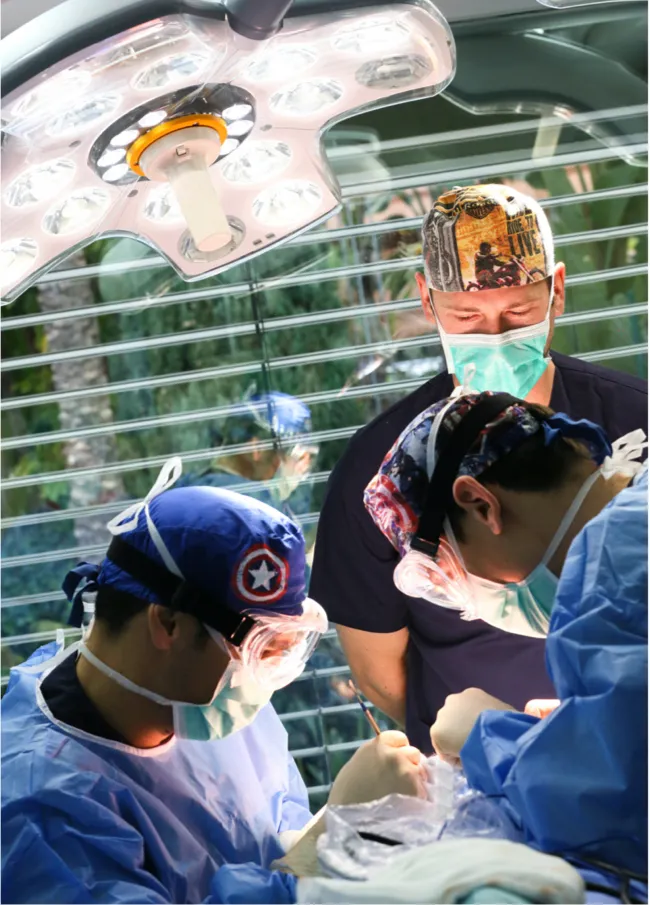
Long-Term Support
Your post-operative journey is crucial, and we’re here to guide you through it. Our dedicated team, comprising esteemed surgeons, attentive coordinators, and a supportive psychologist, remains actively engaged. From scheduled follow-up visits to addressing any concerns that arise, we ensure you’re well-supported and informed.
Unique Offerings
Even after you leave Naghoi, your dedicated Post-Operative Coordinator will remain in contact. We continue to offer virtual support, progress reviews, and access to resources for up to two years post-surgery.
Should any medical revision be necessary, our team will provide it with full transparency and care, reinforcing Facialteam’s commitment to your safety and satisfaction.
Your Post-Op Guide
Knowledge aids recovery. We’ve crafted detailed post-operative instructions to guide you through the recovery process.
Through continuous feedback, we refine our care so that every patient’s experience reflects our highest standard of compassion and professionalism.
Naghoi by Facialteam — Where healing begins and transformation continues.













